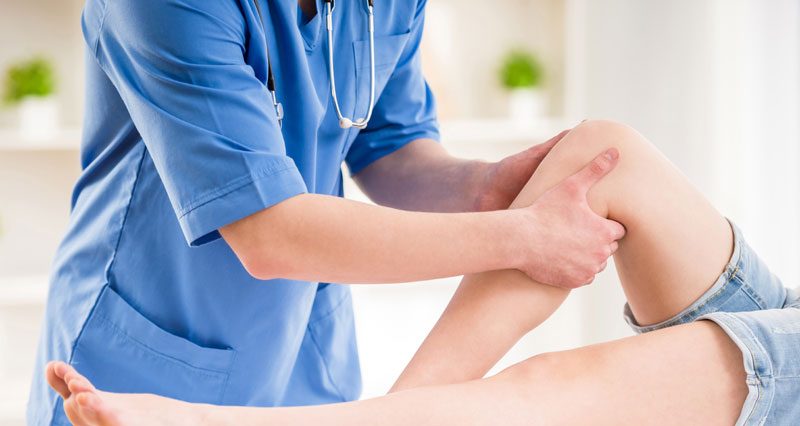
Joint pain has a way of reshaping daily behaviour long before people consciously acknowledge it. Small adjustments creep in, shorter walks, avoided stairs, hesitation when lifting. For some, seeking an orthopedic surgeon in Thailand becomes part of a broader decision to address mobility concerns rather than continuing to compensate quietly.
Travelling for specialist care introduces a different mindset. The physical distance from home often creates mental space to focus fully on the body rather than juggling appointments around work and family schedules. This separation can sharpen attention to symptoms, posture habits, and recovery goals in ways that are harder to achieve during routine domestic care.
The First Consultation Experience
Initial assessments tend to feel more comprehensive when time pressure eases. Movement analysis, imaging review, and hands-on examination combine to build a clearer picture of how joints interact rather than isolating pain to a single area.
Patients often notice that explanations become more visual and demonstrative. Seeing how ligaments move or how alignment affects load distribution makes abstract discomfort easier to understand. This clarity reduces uncertainty and helps individuals participate more actively in treatment decisions.
Navigating Communication and Cultural Nuance
Healthcare abroad introduces subtle cultural differences in communication style. Some patients appreciate the calm pacing and structured explanations, while others adjust to variations in consultation etiquette or follow-up processes.
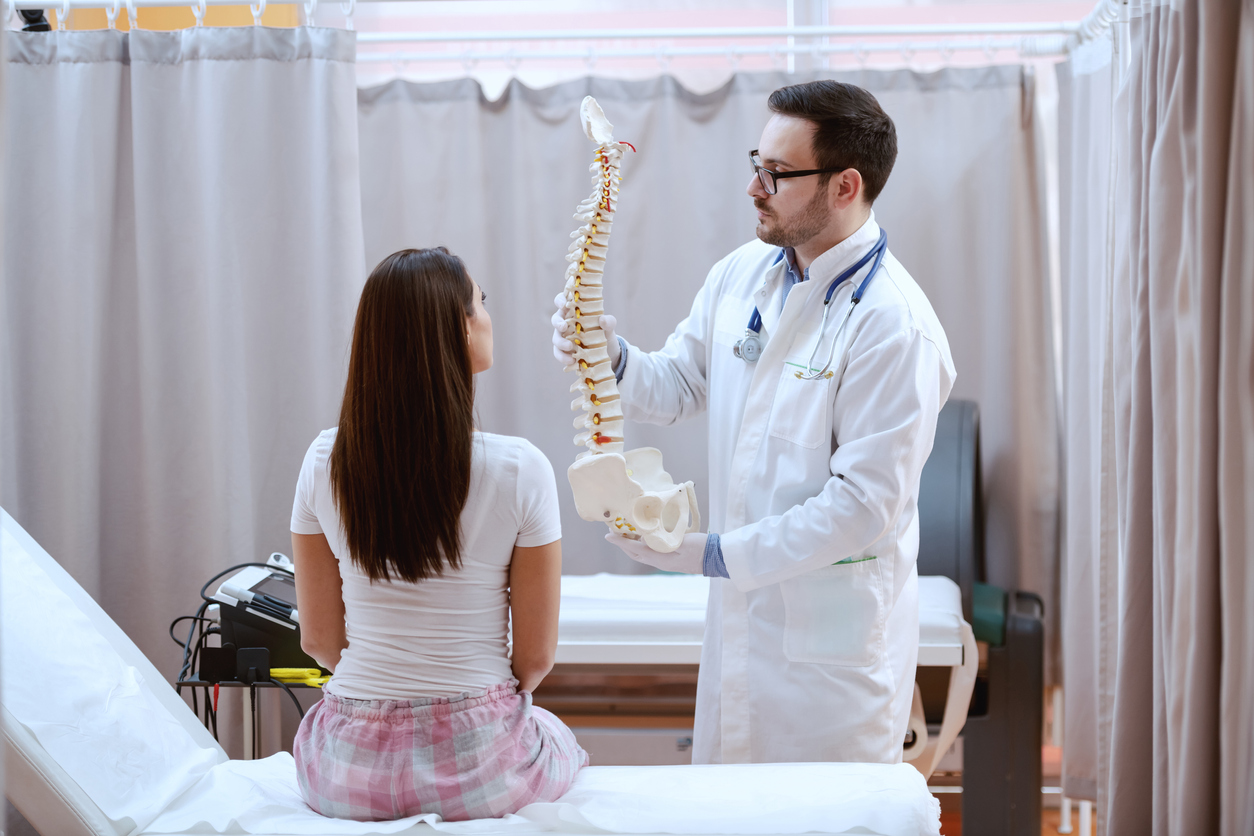
Clear documentation and visual references help bridge these gaps. Many people find that focused, respectful dialogue builds confidence even when communication styles differ slightly from what they are accustomed to at home.
Recovery Away From Routine Pressures
Healing benefits from reduced cognitive load. Being removed from everyday obligations allows rest, gentle movement, and rehabilitation exercises to take priority rather than competing with deadlines and domestic responsibilities.
Patients often become more aware of posture habits, sleep patterns, and hydration when distractions decrease. These small behavioural adjustments support recovery more effectively than isolated clinical interventions alone.
Emotional Shifts During Mobility Improvement
Regaining ease of movement influences mood more than many expect. Reduced pain restores spontaneity, willingness to socialise, and confidence in physical capability. Emotional relief frequently accompanies physical improvement.
This emotional shift reinforces motivation to maintain rehabilitation routines and long-term joint care habits.
Decision-Making Beyond Procedure Type
Choosing specialist care abroad rarely hinges solely on procedure availability. Trust, clarity of explanation, recovery environment, and personal comfort all influence perceived value.
Patients often weigh how supported they feel throughout the process rather than focusing exclusively on technical outcomes.
Long-Term Perspective on Movement Health
Mobility is foundational to independence, social engagement, and emotional wellbeing. Addressing joint issues proactively rather than reactively preserves quality of life across decades.
For many, the experience becomes a turning point in how they treat physical maintenance, shifting from symptom management towards intentional movement care that integrates awareness, consistency, and respect for the body’s limits.
-
Achieving Natural Results: Innovations in Hair Transplant Techniques
October 22, 2023 -
What do clinics for men’s health do?
May 3, 2023
Recent Posts
- The Hidden Dangers of Pod E-Cigarettes May 9, 2026
- Top 6 Treatments Offered by a Cosmetic Dentist London, Explained by Specialists April 20, 2026
- How Singapore Gym Trainers Design Programmes Around Variability Conditioning April 15, 2026
- Why A Good Massage In Bangkok Can Change The Pace Of Your Trip March 31, 2026
- Why A More Thoughtful Approach Often Leads To Better Aesthetic Decisions March 31, 2026
- The Role of Assessments in Supporting Veteran Wellbeing March 5, 2026
- What Happens When Structure Replaces Motivation February 12, 2026
- Hangover Relief to Jet Lag Recovery: Why IV Drips Are a Game-Changer February 12, 2026